Blog
- CATEGORIES:
-
Natural versus Medicated Frozen Embryo Transfer: Benefits, Challenges, and Success Rates

Key Takeaways Natural FET vs medicated FET. A natural FET tracks a woman’s cycle and ovulation, whereas a medicated FET uses hormones to schedule the uterine lining. Natural FET is […]
Men’s Fertility Testing: An Overview of Tests, Results, and Next Steps

Key Takeaways Fertility testing for men explains common tests used to assess male reproductive health. It covers semen analysis, hormone checks, genetic screening, and physical exams. Semen analysis measures sperm […]
How Age Affects Female Fertility: Biological Changes, IVF Success, and Pregnancy Risks

Key Takeaways How age affects female fertility true facts: Fertility in females declines with age, mainly after the early 30s. Egg number and quality decline with age, which increases the […]
Diminished Ovarian Reserve: What It Means for Your Fertility, Symptoms, Testing & Treatment
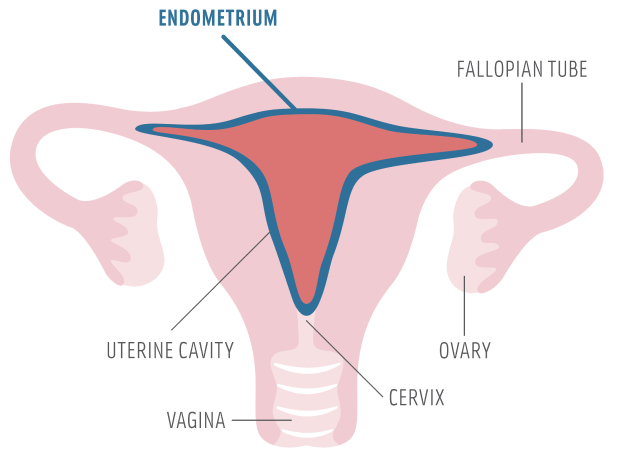
Key Takeaways Diminished ovarian reserve means a reduced quantity and quality of your eggs. It frequently manifests as reduced AMH, reduced follicles on ultrasound or accelerated egg loss with age. […]
Recurrent Miscarriage Testing and Management Plan

Key Takeaways As many as 50% of cases are unexplained. Record all tests, calibrate your expectations, and develop a personalized plan involving medical therapy, assisted reproduction, and psychosocial care. Recurrent […]
Embryo Mosaicism and PGT-A: What It Means for IVF and Future Directions
Key Takeaways Embryo mosaicism PGT-A explained is that certain embryos are classified as ‘mosaic’ – having a mixture of normal and abnormal cells found by preimplantation genetic testing for aneuploidy. […]
The pros and cons of preimplantation genetic testing for aneuploidy (PGT-A)

Key Takeaways PGT-A testing pros and cons are the advantages and disadvantages of preimplantation genetic testing for aneuploidy. It can increase implantation rates and reduce miscarriage risk by testing embryos […]
Fresh vs. Frozen Embryo Transfer: Differences, Success Rates, and Benefits

Key Takeaways Fresh transfer means putting an embryo back into the uterus during the same cycle as the egg retrieval, while FET uses embryos that have been thawed and transferred […]
Recurrent implantation failure: causes, diagnostic workup, and therapeutic strategies
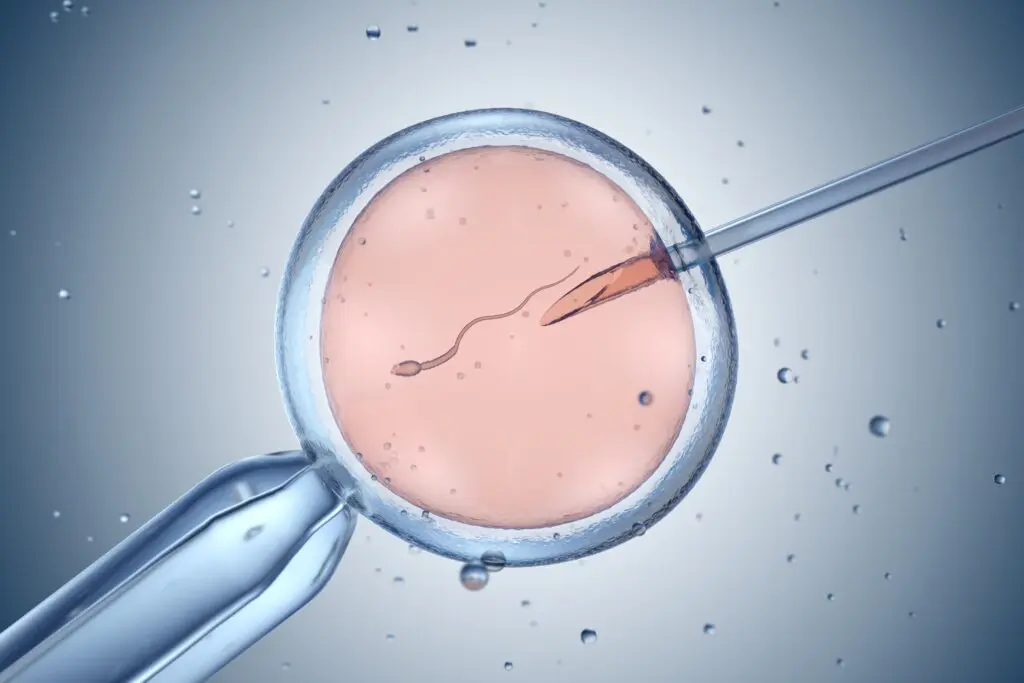
Key Takeaways Recurrent implantation failure workup is the workup used to identify causes when embryos fail to implant after multiple IVF cycles. This can incorporate genetic screening, uterine imaging, immune […]
Time-Lapse Imaging in IVF: Benefits, Limitations, and Patient Impact

Key Takeaways Time-lapse embryo imaging benefits: With this technology, the embryos can be continuously monitored to determine the best possible ones for transfer. The technique captures cell divisions and morphology […]
Artificial intelligence for embryo selection in IVF: roles, advantages, challenges, and future perspectives
Key Takeaways AI embryo selection in IVF is the process of using machine learning algorithms to evaluate embryo images and other data to predict the likelihood of implantation. It integrates […]
ICSI vs. Conventional IVF: Differences, Success Rates, and How to Choose
Key Takeaways ICSI vs conventional IVF are two popular assisted reproduction techniques. ICSI injects a single sperm into an egg and fits severe male-factor infertility or previous fertilization failure. Conventional […]
